
The impact of Hospital-at-Home on the sustainability of the healthcare system
Home hospitalization —also called Hospital-at-Home— emerges as an alternative approach to conventional hospital care, with potential benefits not only for clinical results and patient experience, but also for its impact on the environment. Recent studies show that the partial transition of hospital care to the patient's home can positively influence the reduction of emissions and other environmental impacts associated with traditional hospital care.
Rigorous definition of Hospital at Home

Hospital-at-Home is understood as the provision of active, temporary, and multidisciplinary hospital care in the patient's home, as a total or partial substitution for conventional admission. Hospital-at-Home is a generalist care service mainly of an acute nature that transfers to the patient's home the professionals, equipment, technologies, medicines, and competencies that are usually provided in a hospital through a conventional admission. This hospital care is offered in person and is directed at selected patients, and can be developed in their own home, in a relative's home, or in residential centers. This definition is essential to understand that home hospitalization is not equivalent to basic home care.
The environmental challenge of the healthcare sector and home hospitalization
Although home hospitalization has experienced a notable boost in terms of capacity and visibility —especially during the COVID-19 pandemic—, its widespread adoption continues to face relevant challenges. Recent analyses point out that the impact of Hospital at Home is conditioned by the need to overcome structural barriers, among which stand out funding models, the availability and organization of the workforce, and the definition of sustainable care models. This conceptual precision is essential, since the real value of Hospital at Home depends on its implementation under clinical and organizational standards comparable to those of the conventional hospital.

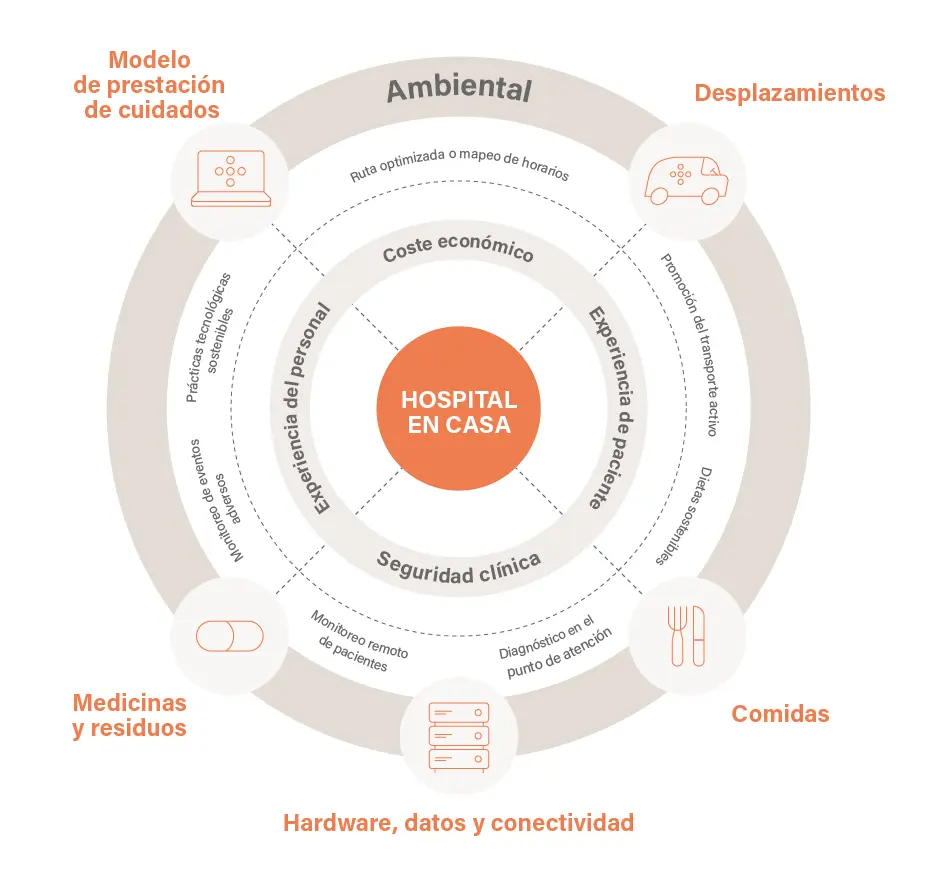
Sustainability and social impact in five areas
1. Food
It can reduce waste and hospital logistics associated with the hospital environment itself. In addition, the impact of Hospital-at-Home is also linked to social impact, by favoring more stable routines and potentially greater well-being in the habitual environment.
2. Clinical Hardware
Hospital-at-Home requires equipment and devices whose manufacture, maintenance, reuse, and transport influence its environmental footprint.
3. Data and infrastructures
Digital infrastructure —clinical platforms, monitoring, and communications— are fundamental for Hospital-at-Home, but consume energy and computational resources. Its impact requires measuring and optimizing this technological layer so that home hospitalization is sustainable also on the digital plane, without assuming unverified environmental benefits.
4. Medicines and waste
Home hospitalization modifies the way medicines are prescribed, administered, and managed, as well as the use of medical material. The Hospital-at-Home model can have a favorable impact by optimizing therapeutic guidelines, reducing waste associated with unnecessary or overdosed treatments, and improving the overall efficiency of the care process. In addition, care at home facilitates greater accompaniment and health education, which translates into better adherence to pharmacological treatments and, consequently, better clinical results and a more responsible use of resources.
5. Care model and travel
The reduction of patient and family travel is usually considered one of the most evident benefits of Hospital-at-Home, with clear implications for sustainability and social impact. The impact of Hospital-at-Home will be conditioned by territorial planning, service capillarity, and the progressive incorporation of autonomous mobility solutions, which could substantially modify transport, logistics, and delivery patterns of home hospitalization.
Current limitations and future steps
Despite its potential, evidence on the impact of Hospital-at-Home remains partial and inconclusive. Systematic evaluation combining environmental perspective with economic and health perspectives through life cycle analysis and standard quantitative methods is required. Likewise, it is necessary to integrate these data into health policies to prioritize investments that maximize benefits of home hospitalization for both patients and the planet.
Awareness to transform the system
Hospital at Home is not only a care alternative; it represents a collective opportunity to rethink how we care for patients, how we finance these needs, and how we sustain a quality healthcare system with guarantees over time. The impact of Hospital at Home goes far beyond the individual patient: it benefits the entire system, the environment, and society as a whole.
For this model to reach its full potential, a shared effort is essential. Regulators, insurance company and mutual executives, health service providers, and, especially relevant, policymakers and the general population must understand that home hospitalization does not subtract care quality, but reinforces it. Raising awareness about these benefits is a common responsibility: every decision, every public policy, and every individual choice constitutes a small grain of sand that contributes to building a more human, more efficient, and also more sustainable healthcare system.

Want to learn more about our services? Visit our services page or contact us directly.
Bibliography
- Powell, D., Burrows, F., Lewis, G. et al. How might Hospital at Home enable a greener and healthier future?. npj Digit. Med. 7, 252 (2024). https://doi.org/10.1038/s41746-024-01249-8
- Society, U. H. A. H. (s. f.). What is HaH. https://www.hospitalathome.org.uk/whatis
- Health care climate footprint report | Health Care Without Harm - Global. (s. f.). https://global.noharm.org/resources/health-care-climate-footprint-report